A Comparison Between Titanium Straight Miniplates Versus Titanium Y Plate in Fixation of Condylar Fracture-A Randomized Clinical Trial
Main Article Content
Abstract
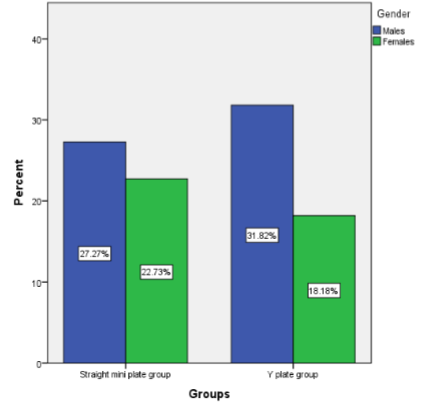
Introduction: Following nasal bone, Mandible comes in the second position in facial fractures. It is fractured in spite of being the strongest and longest bone in the face. Fractures of Mandibular Condyle account for approximately 10%-40% at the time of its comparison with different anatomical sites. Presence of controversy occurs while managing the fractures of condylar. The specific aim of this current study refers to the evaluation of both stability along with complications present in Titanium Straight Miniplate and Y plate in condylar fractures. Materials and Methods: There were a division of 44 patients having condylar fractures into two groups in this specific study. Those specific groups include Straight Mini Plate and Y Plate. There were an evaluation of infection present in the mouth with mouth opening and plate position before one week, month and three months. There were the utilization of “Fisher Exact Test” and “Independent T Test” for assessing the relation in the middle of categorical and continuous variable. Results : The mean age of the patients in straight and Y plate group are 21.45 土 5.67 and 20.98 土 4.23 respectively. Also, 59.09% males and 40.91% females were present in the study. In the patients with Y plates, presence of infection was significantly lower and stability was significantly higher than the control group with straight mini plates. Similarly in the patients with Y plate, mouth opening was significantly higher than the patients with straight plates at p<0.05. Conclusion : Results of satisfactory treatment have been assured by applying Titanium Y Plate in the case of stable osteosynthesis in Condylar fractures. The assurance has been given both by radiological perspective and clinical perspective.
Article Details
References
Choi KY, Yang JD, Chung HY, Cho BC. Current concepts in the mandibular condyle fracture management part I: overview of condylar fracture. Arch Plast Surg. 2012 Jul;39(4):291–300.
Turvey TA. Midfacial fractures: a retrospective analysis of 593 cases. J Oral Surg. 1977 Nov;35(11):887–91.
Valiati R, Ibrahim D, Abreu MER, Heitz C, de Oliveira RB, Pagnoncelli RM, et al. The treatment of condylar fractures: to open or not to open? A critical review of this controversy. Int J Med Sci. 2008 Oct 23;5(6):313–8.
Shi J, Chen Z, Xu B. Causes and treatment of mandibular and condylar fractures in children and adolescents: a review of 104 cases. JAMA Otolaryngol Head Neck Surg. 2014 Mar;140(3):203–7.
Lee J, Jung HY, Ryu J, Jung S, Kook MS, Park HJ, et al. Open versus closed treatment for extracapsular fracture of the mandibular condyle. J Korean Assoc Oral Maxillofac Surg. 2022 Oct 31;48(5):303–8.
García-Guerrero I, Ramírez JM, Gómez de Diego R, Martínez-González JM, Poblador MS, Lancho JL. Complications in the treatment of mandibular condylar fractures: Surgical versus conservative treatment. Annals of Anatomy - Anatomischer Anzeiger. 2018 Mar 1;216:60–8.
Al-Moraissi EA, Ellis E 3rd. Surgical treatment of adult mandibular condylar fractures provides better outcomes than closed treatment: a systematic review and meta-analysis. J Oral Maxillofac Surg. 2015 Mar;73(3):482–93.
Zide MF, Kent JN. Indications for open reduction of mandibular condyle fractures. J Oral Maxillofac Surg. 1983 Feb;41(2):89–98.
Cascone P, Spallaccia F, Fatone FMG, Rivaroli A, Saltarel A, Iannetti G. Rigid versus semirigid fixation for condylar fracture: experience with the external fixation system. J Oral Maxillofac Surg. 2008 Feb;66(2):265–71.
Danda AK, Muthusekhar MR, Narayanan V, Baig MF, Siddareddi A. Open versus closed treatment of unilateral subcondylar and condylar neck fractures: a prospective, randomized clinical study. J Oral Maxillofac Surg. 2010 Jun;68(6):1238–41.
Weiss JP, Sawhney R. Update on mandibular condylar fracture management. Curr Opin Otolaryngol Head Neck Surg. 2016 Aug;24(4):273–8.
Sidebottom AJ. Post-traumatic management of condylar fracture complications. J Oral Biol Craniofac Res. 2022 Mar;12(2):284–92.
Shakya S, Zhang X, Liu L. Key points in surgical management of mandibular condylar fractures. Chin J Traumatol. 2020 Apr;23(2):63–70.
Kanno T, Sukegawa S, Furuki Y, Nariai Y, Sekine J. Overview of innovative advances in bioresorbable plate systems for oral and maxillofacial surgery. Jpn Dent Sci Rev. 2018 Aug;54(3):127–38.
Singh A, Arunkumar KV. Standard 3D Titanium Miniplate Versus Locking 3D Miniplate in Fracture of Mandible: A Prospective Comparative Study. J Maxillofac Oral Surg. 2016 Jun;15(2):164–72.
Mishra N, Thakkar N, Kar I, Baig SA, Sharma G, Kar R, et al. 3-D Miniplates Versus Conventional Miniplates in Treatment of Mandible Fractures. J Maxillofac Oral Surg. 2019 Mar;18(1):65–72.
Sukegawa S, Masui M, Sukegawa-Takahashi Y, Nakano K, Takabatake K, Kawai H, et al. Maxillofacial Trauma Surgery Patients With Titanium Osteosynthesis Miniplates: Remove or Not? J Craniofac Surg. 2020 Jul;31(5):1338–42.
Thomsson M, Johansson B, Krek-manov L. Internal Fixation of Infected Mandibular Fractures with Miniplates ad modum Champy [Internet]. Vol. 2, Journal of Orthopaedic Trauma. 1988. p. 46. Available from: http://dx.doi.org/10.1097/00005131-198802000-00014
Gerlach KL, Schwarz A. Bite forces in patients after treatment of mandibular angle fractures with miniplate osteosynthesis according to Champy. Int J Oral Maxillofac Surg. 2002 Aug;31(4):345–8.
Kozakiewicz M, Swiniarski J. “A” shape plate for open rigid internal fixation of mandible condyle neck fracture. Journal of Cranio-Maxillofacial Surgery. 2014 Sep 1;42(6):730–7.
Ganguly A, Mittal G, Garg R. Comparison between 3D delta plate and conventional miniplate in treatment of condylar fracture: A randomised clinical trial. J Craniomaxillofac Surg. 2021 Nov;49(11):1026–34.
Sikora M, Sielski M, Stąpor A, Chlubek D. Use of the Delta plate for surgical treatment of patients with condylar fractures. J Craniomaxillofac Surg. 2016 Jul;44(7):770–4.
Huang CM, Chan MY, Hsu JT, Su KC. Biomechanical analysis of subcondylar fracture fixation using miniplates at different positions and of different lengths. BMC Oral Health. 2021 Oct 21;21(1):543.
Steed MB. Advances in the Management of Mandibular Condylar Fractures, an Issue of Atlas of the Oral and Maxillofacial Surgery Clinics. Elsevier - Health Sciences Division; 2017.
Zrounba H, Lutz JC, Zink S, Wilk A. Epidemiology and treatment outcome of surgically treated mandibular condyle fractures. A five years retrospective study. J Craniomaxillofac Surg. 2014 Sep;42(6):879–84.
Gualtieri M, Pisapia F, Fadda MT, Priore P, Valentini V. Mandibular Fractures Epidemiology and Treatment Plans in the Center of Italy: A Retrospective Study [Internet]. Vol. 32, Journal of Craniofacial Surgery. 2021. p. e346–9. Available from: http://dx.doi.org/10.1097/scs.0000000000007118
Chaudhary M, Pant H, Singh M, Vashistha A, Kaur G. Evaluation of trapezoidal-shaped 3-D plates for internal fixation of mandibular subcondylar fractures in adults. J Oral Biol Craniofac Res. 2015 Sep;5(3):134–9.
Choi BH, Yi CK, Yoo JH. Clinical evaluation of 3 types of plate osteosynthesis for fixation of condylar neck fractures. J Oral Maxillofac Surg. 2001 Jul;59(7):734–7; discussion 738.
Palani T, Panchanathan S, Rajiah D, Kamalakaran A, Hafeez AA, Raghavan P. Evaluation of 3D Trapezoidal Plates in Open Reduction and Internal Fixation of Subcondylar Fractures of Mandible: A Clinical Trial. Cureus. 2021 Jun;13(6):e15537.
Mohan AP, Jeevan Kumar KA, Venkatesh V. Comparison of preauricular approach versus retromandibular approach in management of condylar fractures. Journal of maxillofacial [Internet]. 2012; Available from: https://link.springer.com/article/10.1007/s12663-012-0350-1
Joevitson DM, Thangavelu DA, Kripakaran DB, Thiruneelakandan D, Janarthanan D, Eshona Pearl D. A new 3D strut plating in management of subcondylar fractures – A prospective study. Saudi j oral dent res. 2020 May 23;05(05):245–9.